Please let me know anything need to be added or updated in the comment box below. If Date of injury not reported within the set deadline, then claims will be denied as failure to report the work related injury on time.ĭate of Injury (DOI): It is the date Injury occurred at work place or illness due to work.Įach state has own timely filing limit to submit the workers compensation claim, also to report an injury and the workers comp time limit list are as follows: Time Limit for filing workers compensation claim - Statewise It is the time for an employee to report work related injury/illness to his employer or supervisor within the set time frame. Time Limit for reporting the Date of Injury: If the claim filed after the time frame, then claim will be denied as past the time filing limit. It is a time frame to submit the claim in order to reimburse the payments from workers compensation insurance from the date of injury occurred. *Currently excludes: UnitedHealthcare commercial and Medicare Advantage Plans of Colorado, Pharmacy, Behavioral Health, Overpayment Reconsiderations & Appeals requests, Capitated and delegated health care professionals, All Savers, Medicare Supplement plan, OneNet PPO, Preferred Care Network, Preferred Care Partners (delegated), Rocky Mountain Health Plan, Sierra Health & Life, Student Resources, Surest (formerly Bind), UnitedHealthcare FlexWork, UHC Global, UHC West, UMR, and UHOne/Golden Rule.Workers Compensation time limit for filing a Claim in United States: Primary Access Administrators may also contact Web Support for help updating notification emails. CT, Monday–Friday.įor help accessing the portal and technical issues, please contact UnitedHealthcare Web Support at or 86, option 1, 7 a.m.–9 p.m. Workers Compensation time limit for filing a Claim in United States: It is a time frame to submit the claim in order to reimburse the payments from workers compensation insurance from the date of injury occurred. Please contact UnitedHealthcare Provider Services at 87, TTY/RTT 711, 7 a.m.–5 p.m. Review the most up-to-date information, exclusions and schedule at /digital. We encourage you to explore our digital solutions and review your workflows so that your team is prepared. We’ll also continue to encourage UnitedHealthcare commercial members to use digital ID cards.Īll required paperless transitions will be announced in Network News at least 90 days prior to the change. Later in 2023, we’ll require you to submit claims and claim attachments electronically. In 2023, you can expect more paper submissions and mailings we send you to go digital. More information can be found in the Network Administrative Guide at /guides. The 2-step process allows for a total of 12 months for timely submission of both steps. Step 2 is to file an appeal if you disagree with the outcome of the claim reconsideration decision. Step 1 is to file a claim reconsideration request. (Claim reconsiderations don’t apply to some states based on applicable state law.) 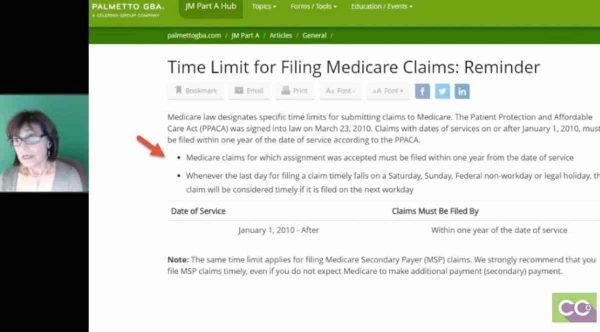 
There is a 2-step process for network health care professionals and facilities if they don’t agree with the outcome of the original claim payment or denial. In the menu, click Claims & Payments > Look up a Claim to search by the claim number and click Act on Claim.If you are a new user and don’t have a One Healthcare ID, visit /access to get started.Sign in to the portal with your One Healthcare ID and password.Go to > Select Sign In at the top-right corner.Please share the following changes and digital workflow options with your team, including outside vendors, such as revenue cycle management companies. This does not affect pre-service clinical appeals. This change affects most* network health care professionals (primary and ancillary) and facilities that provide services to commercial and UnitedHealthcare® Medicare Advantage plan members. 1, 2023, you’ll be required to submit claim reconsiderations and post-service appeals electronically. May make it easier for health care professionals to meet reconsideration and appeal timely filing deadlines by eliminating mail timesĪs a result, beginning Feb.Eliminates postal delays, lost mail, and processing time for UnitedHealthcare to receive and scan the documents into our system.In 2023, our work to replace paper with digital tools will shift to eliminating paper you send to us. Updates: Article now includes additional benefits to digital submissions, reconsideration and appeals-specific training guide, updated instructions for accessing API Marketplace and Medicare Supplement plan exclusion. Affects network commercial and Medicare Advantage health care professionals and facilities
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
